|
4/15/2024 0 Comments Criteria for ptsd in dsm 5 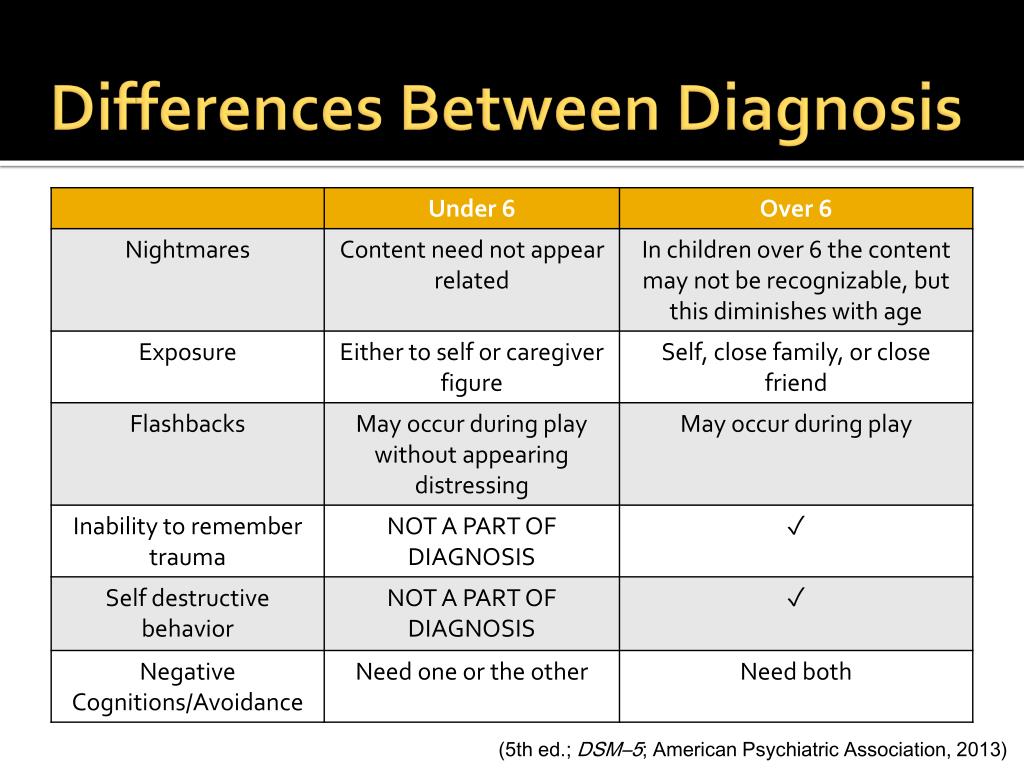
To best help children with PTSD, Herringa said it is important to consider the entire family dynamic, as well as their friends and support network. Research shows that PTSD carries the highest risk of any mental illness of a first-time suicide attempt in young people, so clinicians and family members should stay vigilant to that risk as well as to the risk for self-harm, Herringa said. More than two-thirds of youth with PTSD have a comorbid psychiatric condition (68%), with attention-deficit/hyperactivity disorder the most common, followed by social phobia or other anxiety disorders, and then mood disorders. Unfortunately, there are no evidence-based medications for pediatric PTSD, but medications for comorbid disorders may still be helpful. The strongest evidence base is for trauma-focused cognitive-behavioral therapy eye movement desensitization and reprocessing are also effective. Parents or caregivers are often included, and one important piece involves challenging distorted cognition, including the feelings of guilt about the trauma and that the youth is somehow at fault, Herringa said. Trauma-focused psychotherapy remains the first-line treatment for PTSD in youth and can effectively reduce depressive and anxiety symptoms, Herringa said. However, evidence was not deemed strong enough for its addition to DSM-5. For more than two decades, there has been discussion of creating a new diagnosis, developmental trauma disorder, that is related to multiple and chronic childhood trauma. Herringa said brain imaging research has led to a greater understanding of how children experience PTSD very differently than adults now the DSM-5-TR provides separate diagnostic criteria for children under 7. Since that time the PTSD diagnosis has gradually evolved, and in 1980 DSM-III finally made the illness diagnosable in children. Survivors also reported substance abuse and depression several have since been imprisoned for violence against others. 
Many developed fears of such things as cars, the dark, and the wind and continued to report trauma symptoms even 25 years later. In fact, the children suffered from what is now known as typical PTSD symptoms: panic attacks, nightmares involving kidnappings and death, and personality changes. “Experts at the time thought there would be no lasting effects from this type of trauma,” Herringa said. Miraculously all the students reached the surface safely and were reunited with their families several hours later. The bus driver and an older student worked frantically during the night to dig their way out and move a heavy manhole cover blocking their exit, as the trailer roof began to cave in. Three men hijacked a school bus at gunpoint, drove it 100 miles away, and forced the bus driver and 26 children down a hole into an old trailer that had been buried 12 feet underground. It was a school bus kidnapping in Chowchilla, Calif., in 1976 that changed the long-held notion that children were resilient to trauma, Herringa said. 
Put together, recent imaging studies show a “fairly consistent pattern of developmental decline in adaptive or healthy functioning in the brain, particularly in the emotional regulatory and threat response systems,” Herringa said, adding that more study is needed. That connectivity is critical in helping regulate emotional responses and allowing youth to benefit from exposure therapy, he added. Other brain imaging research by Herringa and others that followed youth aged 8 to 18 has uncovered other differences: Over time youth with PTSD experience regression in normal brain development, namely decreased hippocampal volume, increased amygdala activation, and decreasing prefrontal-amygdala connectivity. In fact, researchers found that the brains of girls exposed to abuse may habitually utilize threat-related circuitry, even when they’re in a safe setting. BBRF is the world’s largest private funder of mental health research.īrain scans of girls who had suffered abuse showed delayed maturity in the emotion circuitry of their brains, which was associated with increased hyperarousal symptoms, one of the hallmarks of PTSD, according to a study by Herringa and colleagues in The American Journal of Psychiatry in 2021. As such, effective recovery from pediatric PTSD may involve helping youth restore their brain’s threat circuitry and executive function, Ryan Herringa, M.D., Ph.D., director of the Division of Child and Adolescent Psychiatry at the University of Wisconsin School of Medicine and Public Health, said at a webinar hosted by the Brain & Behavior Research Foundation (BBRF).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
